To make a diagnosis of epilepsy, your doctor will have to ask a lot of questions (history taking), some preferably from an eye witness who can describe the event(s). This is very important because there are other diseases that may look like seizures but are not actually seizures. Sometimes a video recording of the event may be helpful in arriving at a diagnosis. Epilepsy is a clinical diagnosis, hence there is no single investigation that is diagnostic. However, an electroencephalograph (EEG) and magnetic resonance imaging (MRI) of the brain is helpful in supporting the diagnosis of epilepsy.
A person must have had at least two episodes of unprovoked seizures which are up to twenty-four hours apart before the diagnosis of epilepsy is entertained. Unprovoked here means that the person has not been exposed to any circumstances or substances that may cause a seizure in an otherwise healthy person. Therefore, an individual who has a seizure after falling from a height, following a road traffic accident or after illicit substance use for instance is said to have had a ‘provoked seizure’.
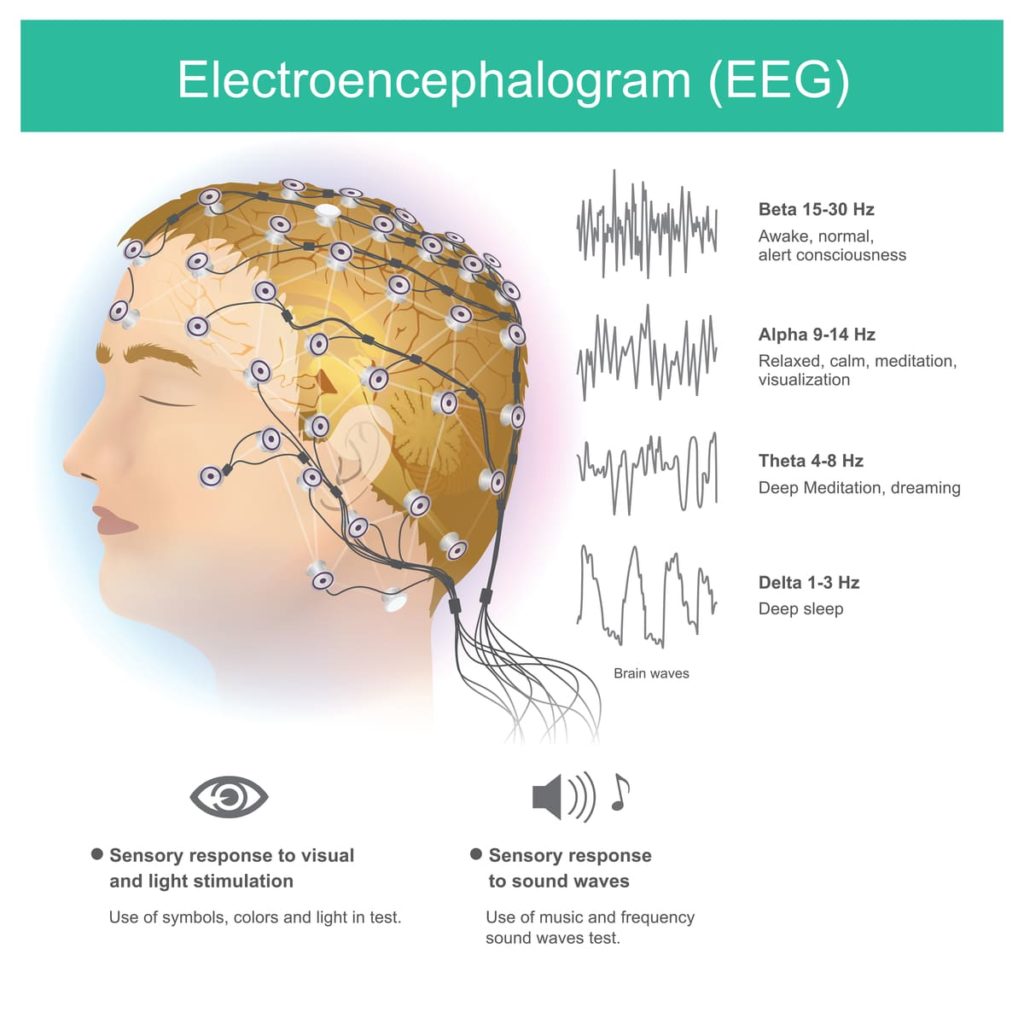
What is electroencephalograph (EEG) and how is it used in the diagnosis of epilepsy?
An EEG though an important investigation, has a low sensitivity and high specificity for the diagnosis of epilepsy. This means that a normal EEG recording does not rule out epilepsy as a diagnosis because the yield of epileptiform activity in a single routine 30- 45 minutes EEG is very low.

Some procedures can help to make abnormal waves on the EEG more obvious. These are done before and during EEG recording and may help to improve the sensitivity of EEG as a supportive diagnostic aid. Activation procedures include sleep deprivation, hyperventilation and photic stimulation.
Therefore, if abnormal waves or epileptiform activity is noted during an EEG recording, it is highly specific for and supports the diagnosis of epilepsy, but the absence of epileptiform activity does not negate the diagnosis of epilepsy. It only means there was no epileptiform activity within the time the EEG recording was obtained. An EEG is also useful in differentiating between a focal and generalized epilepsy. It can show which area of the brain the epileptogenic focus is located at in focal seizures.
A brain MRI is important for the identification of structural brain lesions (eg congenital malformation or scarring in the brain following an insult like infection or trauma) which may be a focus for the generation of epileptiform activities. A brain MRI may also identify a tumour (as a cause of seizure) which may be removable without causing major disabilities.
Usually, your doctor may request other blood tests to have a baseline before the commencement of AEDs as some of these drugs may have some negative effects on your blood counts and serum electrolytes. Blood tests are also useful to identify some metabolic and genetic abnormalities that may be a cause of epilepsy.