What is insulin?
Insulin is a hormone made in your pancreas. The pancreas is a gland behind your stomach that helps with digestion. It helps your body use glucose for energy. When the amount of glucose is high in the bloodstream, the pancreas senses this and releases the right amount of insulin to help drive glucose into your cells where it’s broken down to produce energy that fuels your body.
How does insulin work?

When you have diabetes, it means your pancreas doesn’t make any insulin or doesn’t make enough insulin or the insulin it makes doesn’t work properly. If you need to take insulin as a medication to help you control your blood sugar levels, you are said to be an insulin-dependent diabetic.
Insulin cannot be taken orally because if taken orally, it would break down in the stomach and not get to the bloodstream which means it won’t have any effect. This means it must be injected it or use an insulin pump so that it can enter your bloodstream. If you took it in tablet form, it would be broken down in your stomach and never make it to your bloodstream. Your doctor will tell you if insulin is the right medication for you and you can both agree on the type of insulin you need, when to take it and how much you need to take.
Insulin Pens
Some people with diabetes use insulin pen to inject insulin. The insulin pens makes it easier to administer insulin and allow for a more accurate, convenient and safe delivery than using a vial and syringe.

Parts of an insulin pen
Insulin pen comprises of the
- Cap
- Cartridge holder
- Cartridge
- Pen body
- Screw
- Dose indicator
- Dose window
- Dose knob
- Needle
- Needle shields (inner and outer)
- Paper tab

Types of Insulin Pens
Insulin pens can be categorised into two types.
- Disposable pen-This is disposed of after use.
- Reusable pen-The cartridge can be replaced and re-used.
Insulin vials (insulin bottles)
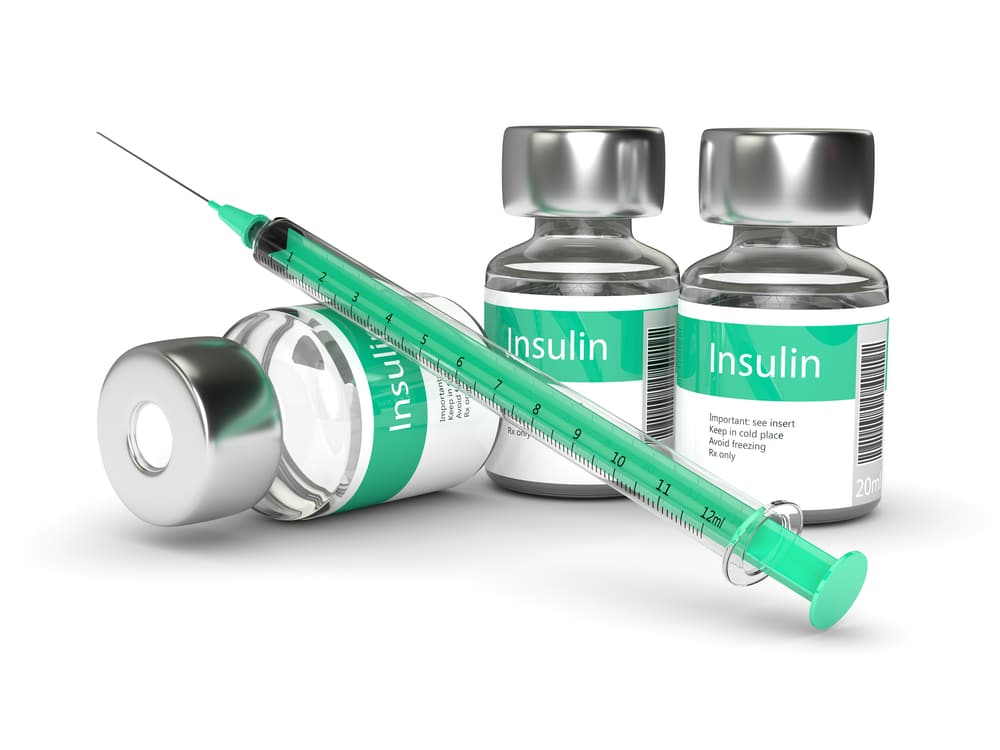
Insulin injections
You need the following to be able to inject insulin safely.
- An insulin pen – it may either already have insulin in it or one where you have to change the insulin cartridge yourself.
- Your needle – this is very small and thin. This is for single use only.
- A sharps bin or needle clipper – this is where you should throw your needle.
Insulin needle (Syringe for insulin)
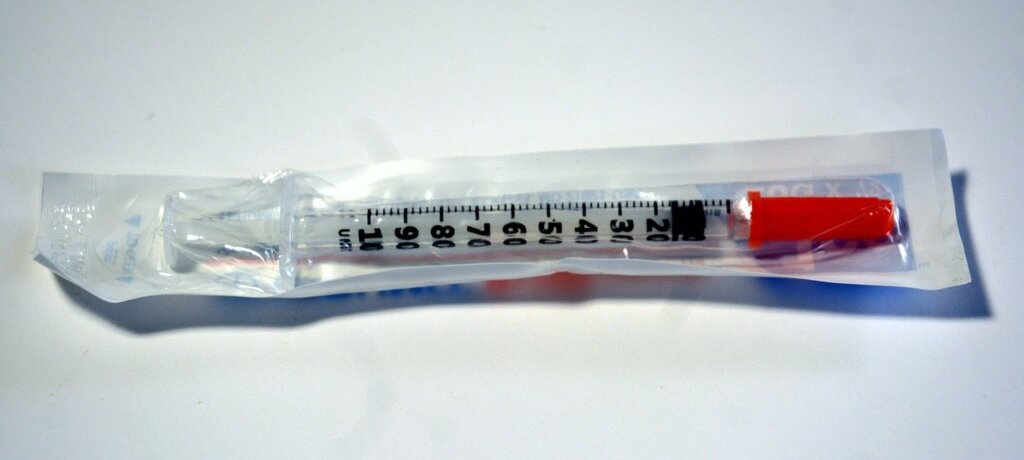
How to inject insulin
Wash your hands with soap and water before injecting. Remember to also dry your hands.
- Choose where you’re going to inject. Look for fatty tissues.
- Attach a new needle onto your pen.
- Remove the outer and inner caps of the pen needle.
- Hold the pen upright and perform an ‘air shot’. This involves you dialling up at least 2 units, pointing the pen upwards and pressing the plunger to expel a test shot of insulin. This priming helps to clear any air bubbles out of the needle.
- Dial up your dose.
- Put the needle in at a right angle (90° angle) and keep the pen steady.
- Press the plunger relatively slowly to inject the dose and wait till the dial goes back to 0
- Leave the needle in for at least 10 seconds to help insulin get into your body and prevent any of the dose escaping out.
- Ensure that the used needle is deposited into a sharps bin or needle clipper.

Where is insulin injected?
The four main diabetic injection areas are thighs, stomach, arms and bum. Insulin should be injected right underneath the skin and not into a muscle or vein.

Insulin pump
An insulin pump is a battery-operated device that releases insulin regularly throughout the day. It’s can be used instead of injecting insulin.

Regimens and Therapies
- Multiple-dose injection regimen is also known as the basal/bolus regime. This involves injecting short-acting or rapid-acting insulin analogue, before meals and intermediate-acting or long-acting insulin, once or twice daily as a basal (background) dose.
- Using a mixture of short-acting or rapid-acting insulin analogue with intermediate-acting or long-acting insulin twice daily before breakfast and dinner
- Using Intermediate-acting or long-acting insulin, once or twice daily with or without short-acting or rapid-acting insulin before meals
- Continuous subcutaneous infusion using an insulin pump.
Insulin Resistance
Insulin resistance is when your body cannot use insulin properly. Insulin resistance is when cells in your liver, muscles and body fat and start resisting or ignoring the signal that the hormone insulin is trying to give out—which is to drive glucose out of the bloodstream and into our cells. This can lead to a rise in blood sugar levels.

How Insulin Resistance Develops
Genetics, ethnicity and age can be a factor to developing insulin sensitivity. The risk factors for developing insulin resistance include excess body weight, especially too much belly fat, smoking, sleep issues and lack of exercise. At first your body responds by producing more insulin. Over time, the beta cells in your pancreas that are working so hard to make insulin get worn out and can no longer keep pace with the demand for more and more insulin and your blood sugar may begin to rise.
Symptoms of insulin resistance
Insulin resistance does not usually show any signs and symptoms. It is usually when it has led to other conditions like high blood sugar levels that symptoms appear. Some of these symptoms include:
- Tiredness (lethargy)
- Hunger
- Difficulty with concentration
Signs of insulin resistance
- High blood pressure
- High cholesterol
- Belly fat
Types of insulin
There are five different types of insulin and they all work a little bit differently. You will decide which one is best for you with the help of your doctor.
Rapid-acting insulin
Rapid-acting insulin also known as fast-acting insulin shortly before or after meals to cover the blood glucose elevation from eating. This type of insulin works very quickly and is usually taken with an intermediate-acting insulin or long-acting insulin. Example is Aspart (Novorapid), Glulisine (Apidra), Lispro (Humalog).

Short-acting insulin
Short-acting insulin is like rapid-acting insulin but is a little bit slower to act. As a result of being slower, it is usually taken around 30 minutes before food to cover the blood glucose elevation from eating. It is also called a bolus insulin. Example is Actrapid, Humulin S, Insuman Rapid.
Mixed insulin
This is a mixture of short-acting insulins and long-acting insulins. You still take it before meals, but you won’t have to take a background insulin as well. Example is Novomix 30, Humalog Mix 25, Humulin M3
Intermediate-acting insulin
Intermediate-acting insulin is also known as background insulin or basal insulin. It works to reduce the blood glucose elevations when rapid-acting insulins or short-acting insulin stops working. This type of insulin is often used together with rapid- or short-acting insulin and is usually taken once or twice a day. Example is Isophane/NPH (Insulatard, Humulin I, Insuman Basal)
Long-acting insulin
Long-acting insulin is like intermediate insulin only that it is slower acting. It works to reduce the blood glucose elevations when rapid-acting insulins or short-acting insulin stops working. This type of insulin is often used together with rapid- or short-acting insulin and is usually taken once a day at the same time each day. Example is Detemir (Levemir), Glargine (Absaglar, Lantus), Degludec (Tresiba)
| Type | Brand Name | Onset (length of time before insulin reaches the bloodstream) | Peak (time period when insulin is most effective) | Duration (how long insulin works for) |
| Rapid-acting | Humalog Novolog Apidra | 10 – 30 minutes | 30 minutes – 3 hours | 3 – 5 hours |
| Short-acting | Regular (R) | 30 minutes – 1 hour | 2 – 5 hours | Up to 12 hours |
| Intermediate- acting | NPH (N) | 1.5 – 4 hours | 4 – 12 hours | Up to 24 hours |
| Long-acting | Lantus Levemir | 0.8 – 4 hours | No peak or minimal peak | Up to 24 hours |
Side effects of insulin
Hypos
Hypos are the most common side effect of taking insulin. Hypos are when your blood sugar is low. This may happen if take too much insulin. If you’re having a lot of hypos, you may be on the wrong dose of insulin and you should see your doctor so that he/she could prescribe you the right dose. Clinical features of hypos include tremors, hunger, sweating etc.
General side effects
flu-like symptoms, headaches and nausea are side effects you may experience within the first 72 hours of starting any new insulin. Consult your doctor for advice if this happens.
Injection site reactions
You can experience itching, rashes or lipoatrophy if you keep injecting on one spot. Lipoatrophie are hard lumps that can form in your injection site and can stop the insulin from working properly. Try and inject in different spots each time you inject.
Weight gain
Taking insulin may cause you to put on weight. There are many reasons why this may happen. Your diet, type of insulin you are prescribed or the amount of insulin you are taking might affect your weight. Human or animal insulin are more likely to make you add weight than analogue insulins. Taking more insulin than you need can make you put on weight. Insulin is a growth hormone, and like any growth hormone you take, you will put on weight.
Overdose
Insulin overdose can be very serious as it can lead to severe low blood sugar levels and in some situations can cause disorientation, seizures and even death. Taking more insulin than you need can lead to insulin overdose. If you accidentally take too much insulin, then immediately eat a lot of fast-acting carbohydrates such as sweets or glucose tablets. You should contact your doctor if you have taken a lot more insulin than you need.
How to store insulin
Keep any insulin you’re not using in the fridge but not freezer as it may damage the insulin if kept in the freezer. Any insulin left out of the fridge for 28 days or more will need to be thrown away as it would have broken down.
The temperature you should store your Insulin should be lower than 25°C (77°F). Ideally, it should be stored between 2 to 6°C (36 to 43°F). Room temperatures may be below 25°C, but it can be higher on hot days so it’s best to keep your insulin in the fridge.
Always read the information leaflet to know how to store your insulin as some may need to be stored in a different way.
How insulin is made
Human insulin
This is synthetic insulin made in a laboratory to mimic insulin made by humans. It is created by growing insulin proteins within E-coli bacteria (Escherichia coli).
Analogue Insulin
This insulin is a subgroup of human insulin. Analogue insulins have the same chemical structure of human insulin but have been genetically altered to make it either rapid acting, longer acting or more uniformly acting form of the insulin.
Animal insulin
Just like the name suggests animal insulin is taken from the pancreases of animals, usually pigs (porcine or pork insulin) and cows (bovine or beef insulin). This is not commonly used anymore but some find that animal insulin works better for them.
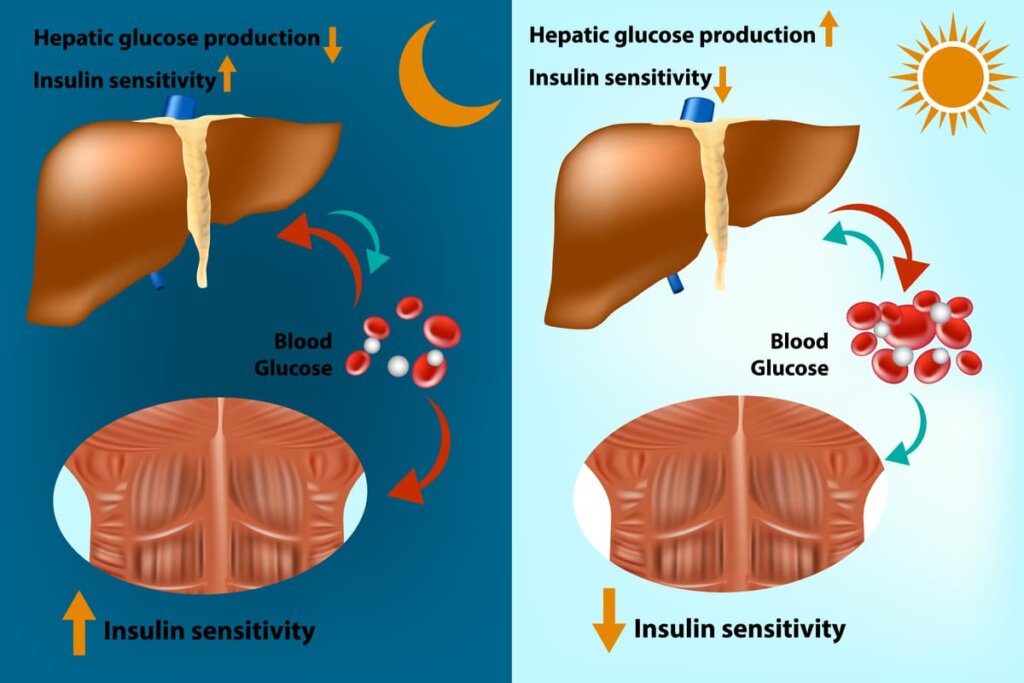
Insulin Sensitivity and your dose
Insulin sensitivity is used by healthcare professionals to describe how well your body is using insulin to reduce your blood sugar. Someone with high sensitivity will need less insulin to lower blood glucose levels than those with low sensitivity. Insulin sensitivity varies from one person to another and your doctor can test you to determine how sensitive you are to insulin. This can help them decide what dose of insulin you would require or if you even require insulin at all.
Frequently asked question
Where is insulin produced in the body?
Insulin is produced in the pancreas. See above to see how it does it.
Where is insulin injected?
Insulin is usually injected on thighs, stomach, arms and bum. See picture on above.
What does insulin do?
Insulin helps drive glucose into your cells where it’s broken down to produce energy that fuels your body.
Is insulin a hormone?
Yes, insulin is a hormone produced by the pancreas.
